More Interesting Blogs & Tips on Physiotherapy & Rehabilitation
Physiotherapy isn’t just for injury recovery – it plays a vital role in maintaining long-ter...
sgpadmin
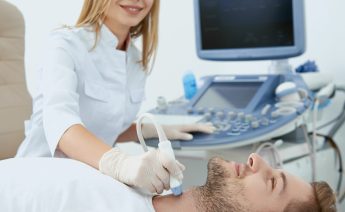
When you’re in pain, getting the right diagnosis quickly makes all the difference. Traditional ass...
sgpadmin
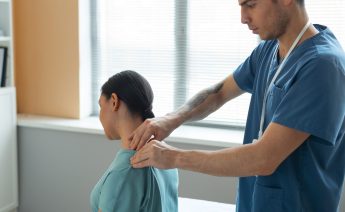
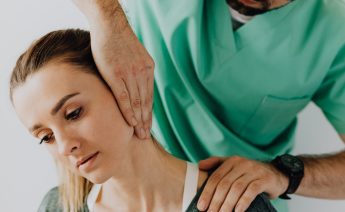
Shoulder pain is one of the most common reasons people seek physiotherapy. From sports injuries to e...
sgpadmin
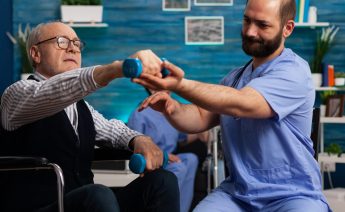
Chronic pain and inflammation can limit mobility, disrupt sleep, and affect your quality of life. Wh...
sgpadmin
Whether you’re a weekend runner, football enthusiast, or competitive athlete, staying injury free ...
sgpadmin
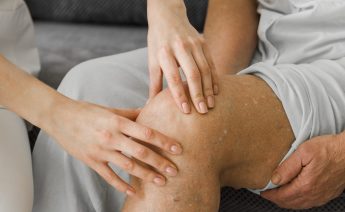
Joint pain can affect everything from walking and climbing stairs to enjoying sports and hobbies. Wh...
sgpadmin
Arthritis affects millions of people worldwide, often leading to stiffness, swelling, and persistent...
sgpadmin
Recovering from surgery isn’t just about healing the wound – it’s about regaining strength...
sgpadmin
When it comes to musculoskeletal (MSK) injuries, an accurate diagnosis is the foundation of effectiv...
sgpadmin
Frozen shoulder, also known as adhesive capsulitis, is a painful condition that restricts movement i...
sgpadmin
When recovering from an injury, building strength, balance, and mobility is essential. At Southgate ...
sgpadmin
Living with chronic pain can feel overwhelming, especially when symptoms persist for months or even ...
sgpadmin
Osteoarthritis (OA) is one of the most common causes of joint pain and stiffness, particularly in th...
sgpadmin
Expert Diagnosis, Rehabilitation & Ultrasound Imaging at Southgate Physio Running is one of the ...
sgpadmin
Southgate Physio’s Expert Support – In Clinic and at Home Undergoing a hip or knee replaceme...
sgpadmin
Why Lower Back Pain Is So Common Lower back pain affects millions of people and is one of the leadin...
sgpadmin
A Southgate Physio Approach Including Ultrasound-Guided Injections (USGI) Shoulder pain is one of th...
sgpadmin
Accurate MSK Assessment and Advanced Ultrasound-Guided Solutions in North London When you’re d...
sgpadmin
When you’re dealing with pain, injury, or mobility issues, choosing the right healthcare profe...
sgpadmin
At Southgate Physio, we are committed to offering cutting-edge care that accelerates healing, restor...
sgpadmin
People of all ages often suffer from knee discomfort, which frequently makes everyday activities and...
sgpadmin
Back pain is one of the most common reasons people seek medical and physiotherapy care. It can stem ...
sgpadmin
When it comes to your health and recovery, choosing the right physiotherapy clinic can make all the ...
sgpadmin
Rotator cuff surgery is a precise procedure aimed at repairing damaged tendons in the shoulder. Howe...
sgpadmin
Although recovering from knee replacement surgery can seem overwhelming, you can regain your strengt...
sgpadmin
Tennis elbow, or lateral epicondylitis, is a painful condition caused by overuse or repetitive strai...
sgpadmin
It’s normal to be interested or perhaps a little nervous about what to expect from your first ...
sgpadmin
At Southgate Physio Clinic in North London, we’re committed to providing effective, evidence-based...
sgpadmin
Sciatica is a painful condition that can significantly impact daily life. It happens when there is i...
sgpadmin
Shoulder pain is a frequent problem that can affect people of all ages, impairing daily activities a...
sgpadmin
Foot health and strength are essential for general mobility and well-being. For individuals who enga...
sgpadmin
Effective treatment starts with a precise diagnosis, especially for musculoskeletal disorders like b...
sgpadmin
Neck pain can be debilitating and interfere with day-to-day activities. If you’re thinking abo...
sgpadmin
Everyday life can be disrupted by shoulder pain, which can make even small chores seem daunting. Res...
sgpadmin
Anyone, from office workers to athletes, can have neck pain, which is a widespread problem. It may b...
sgpadmin
Back pain is one of the most common complaints among people of all ages, often affecting mobility an...
sgpadmin
Whether from overuse, chronic illnesses like arthritis, or injuries, knee discomfort is a frequent p...
sgpadmin
We at Southgate Physio are aware that not everyone is able to attend physiotherapy treatments in a c...
sgpadmin
Foot injuries are a prevalent problem that can have a big effect on our day-to-day activities. Anybo...
sgpadmin
It’s essential to keep your shoulders strong and mobile for everyday tasks and general health....
sgpadmin
Plantar fasciitis can be a debilitating condition, causing heel pain that affects daily activities a...
sgpadmin
ACL injuries are a major worry for those who are physically active and athletics. At Southgate Physi...
sgpadmin
Rotator cuff tears are a common shoulder injury that can lead to significant pain and functional imp...
sgpadmin
Achilles tendon ruptures are debilitating injuries that can significantly impact mobility and qualit...
sgpadmin
At Southgate Physio, we are committed to providing our patients with the latest and most effective t...
sgpadmin
Plantar fasciitis can be a debilitating condition, causing heel pain that affects daily activities a...
sgpadmin
Here at Southgate Physio, which is in North London, we use the cutting-edge method of ultrasound-gui...
sgpadmin
At Southgate Physio a Private Physiotherapy Clinic, we’re dedicated to giving our patients the...
sgpadmin
Degenerative disc disease (DDD) is a common condition that affects the spine and can cause significa...
sgpadmin
Soft tissue injuries are frequently sustained due to a variety of activities, including sports, acci...
sgpadmin
As part of our dedication to offering individualised care and customised treatment programmes, we at...
sgpadmin
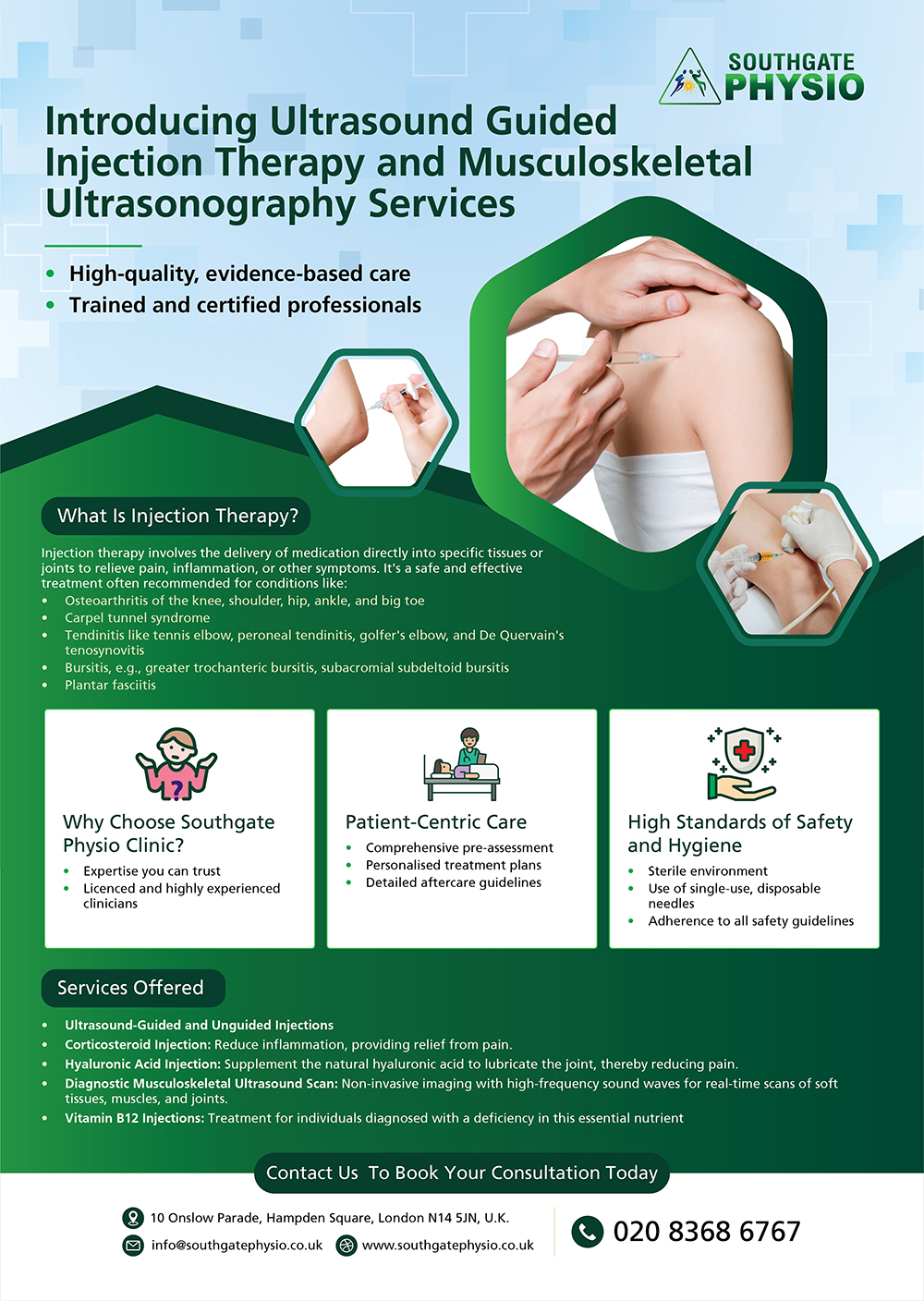
We are excited to introduce Injection Therapy and Musculoskeletal Ultrasonography services at Southg...
sgpadmin
At Southgate Physio, we understand how debilitating Tensor Fasciae Latae (TFL) pain can be. The musc...
sgpadmin
Osteoarthritis makes daily living difficult and can impair comfort, movement, and general well-being...
sgpadmin
Pain in the sacroiliac joint can be quite incapacitating, impairing one’s movement, comfort, a...
sgpadmin
One’s quality of life can be greatly impacted by chronic pain, which can also have an adverse ...
sgpadmin
Technological developments in the field of medical diagnostics are constantly changing the way we ap...
sgpadmin
For athletes of all levels, sports injuries can be a frequent and frustrating occurrence. Whether yo...
sgpadmin
Hyaluronic acid is a remarkable substance known for its multifaceted benefits, from promoting skin h...
sgpadmin
Millions of people worldwide suffer from musculoskeletal disorders (MSDs), which include pain and im...
sgpadmin
Tennis elbow, sometimes referred to as lateral epicondylitis, is a painful ailment that affects the ...
sgpadmin
At Southgate Physio Clinic, we frequently encounter patients whose lives have been momentarily disru...
sgpadmin
A successful fitness regime often lies in the simplicity of the exercises it incorporates. Among the...
sgpadmin
As healthcare providers dedicated to alleviating discomfort and promoting functional well-being, the...
sgpadmin
Physiotherapy encompasses a wide range of specialties, all of which work to promote healthy movement...
sgpadmin
The menisci are two C-shaped pieces of cartilage that sit between your shinbone and thighbone and se...
sgpadmin
Although many people are affected by bursitis, which is a disorder that is not well-known outside of...
sgpadmin
Even though Diastasis Rectus Abdominis (DRA) may not be a well-known ailment, it affects a lot of pe...
sgpadmin
Your shoulder’s acromioclavicular joint, also known as the AC joint, is an essential component...
sgpadmin
Chronic pelvic pain is a common problem and presents a significant challenge to healthcare providers...
sgpadmin
If you’re struggling with pain, you may be searching for effective methods to manage your symp...
sgpadmin
Shoulder discomfort can cause inconvenience and hinder your day-to-day tasks. The good news is that ...
sgpadmin
Physiotherapy is a form of treatment that involves the use of physical methods such as exercise, mas...
sgpadmin
Acute neck pain is more common than you think. According to research, up to 70% of adults will exper...
sgpadmin
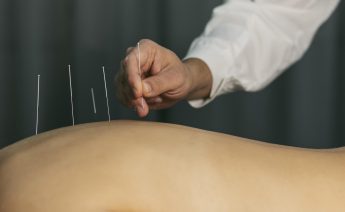
This blog explores the ancient practise of acupuncture in Chinese medicine, which has stood the test...
sgpadmin
Consider using manual physiotherapy if you’re looking for an effective way to manage your chro...
sgpadmin
Manual physiotherapy is a crucial aspect of physiotherapy that involves hands-on techniques to diagn...
sgpadmin
Shoulder impingement is a common physical ailment that compresses the rotator cuff tendons, causing ...
sgpadmin
Tennis elbow, clinically known as lateral epicondylitis, is a common condition that affects not only...
sgpadmin
Plantar fasciitis is a common condition characterised by pain and inflammation in the plantar fascia...
sgpadmin
Arthritis affects millions worldwide and may significantly restrict their everyday lives by producin...
sgpadmin
Surgery could be the most critical part of the treatment process; however, this is true that Post-su...
sgpadmin
Physiotherapy and exercise are typically first-line treatments for acquiring relief from pain whilst...
sgpadmin
The new age of working has given rise to occasional neck pain and stiff neck. Almost two-thirds of p...
sgpadmin
The modern-day lifestyle has caused many individuals to be more prone to experiencing musculoskeleta...
sgpadmin
An elbow fracture causes stiffness, resulting in a reduction in the range of motion and functioning ...
sgpadmin
Have you ever lost balance and suffered a foot twist whilst landing? Well, we’ve all been ther...
sgpadmin
Millions of people suffer from work-related musculoskeletal disorders every year. As per studies, ar...
sgpadmin
Welcome to our blog about advanced physiotherapy. Here, we will talk about the advantages and method...
sgpadmin
Did you know that osteoporosis causes around 1.5 million spinal compression fractures annually in th...
sgpadmin
Low back pain is one of the leading health concerns of the present, especially due to our sedentary ...
sgpadmin
Pregnancy is one of the most beautiful phases and needs expert-level care. Antenatal care is one of ...
sgpadmin
If you are experiencing any physical discomfort or pain and want to seek the help of a physiotherapi...
sgpadmin
Lifelong happiness requires consistent efforts towards maintaining optimal physical well-being. Ther...
sgpadmin
Shoulder health can be greatly improved by incorporating scapular retractions into your fitness and ...
sgpadmin
Tennis elbow occurs as a result of inflammation or injury to the common extensor origin at the Elbow...
sgpadmin
Physical exercise gains greater significance as we grow older. Older individuals can benefit signifi...
sgpadmin
Is acupuncture the miracle remedy for everything? For those new to holistic treatment, acupuncture c...
sgpadmin
Definition of Frozen Shoulder Adhesive capsulitis, also known as frozen shoulder, is a medical condi...
sgpadmin
Modern work routines have undergone a seismic shift whilst transforming the pattern of working. It h...
sgpadmin
Extracorporeal shockwave therapy (ESWT), commonly known as shockwave therapy, is a minimally invasiv...
sgpadmin
Frozen shoulder is a medical condition in which a person experiences pain and stiffness in the shoul...
sgpadmin
Pilates is a joyous mind-body exercise that is now well recognised worldwide for its promising healt...
sgpadmin
Tensor Fascia Latae or TFL is a small muscle located on the top of the hip in the human body. It hel...
sgpadmin
Traditionally, physiotherapists have primarily been associated with rehabilitation and recovery from...
sgpadmin
Muscle strain is one of the most common types of overuse injury, especially among athletes. It occur...
sgpadmin
A runner’s foot constantly endures the brunt of repetitive bashing up to three to seven times the ...
sgpadmin
Southgate Physio is one of the most reliable Physiotherapy clinics in North London. We offer a wide ...
sgpadmin
One of the most concerns among people regarding their knees is a strange clicking sound when extendi...
sgpadmin
Osteoarthritis is one of the leading causes of knee pain and manifests as chronic pain, swelling, an...
sgpadmin
Modern lifestyle and intensive workout regimes have made us extremely adept at scapular protraction ...
sgpadmin
Tech neck is the fallout from the increased dependence on smartphones and computers and the poor pos...
sgpadmin
Physiotherapy is an essential treatment form for thousands of individuals across the UK today. Those...
sgpadmin
A branch of rehabilitative health, physical therapy makes use of uniquely designed exercises to help...
sgpadmin
Ligaments, tendons and muscles are referred to as soft-tissues. Sometimes they become injured or str...
sgpadmin
Pain is an annoyance and that is not a secret. It can hinder your overall quality of life. Medicatio...
sgpadmin
Physiotherapy takes a holistic approach to healing. It goes beyond one condition or injury and consi...
sgpadmin
Are you struggling with muscle aches and strains? Do you want to recover faster from training and re...
sgpadmin
Physiotherapy treatment is typically used as a part of a rehabilitation or recovery plan. People usu...
sgpadmin
The days of only elders complaining of back and neck pains are gone. Today, school-going children, t...
sgpadmin
Physiotherapy can be a transformative experience and people of all ages can take advantage of it. Ph...
sgpadmin
Pilates is not just any workout. People who have been practicing it for some time now understand tha...
sgpadmin
After having a baby, your body shape and size might change. If you are a new mother and worrying abo...
sgpadmin
For regular runners, especially those training for marathons or other such events, one of the greate...
sgpadmin
Back pain happens to be one of the main reasons why people miss work or go to the doctor. It is the ...
sgpadmin
Physiotherapy is one of the most widely-used treatment modalities for countless individuals today. M...
sgpadmin
Sports injuries can be quite distressful from a physical as well as mental standpoint. Any athlete w...
sgpadmin
Gone are the days when grandparents complained about aches and pains. Nowadays, teenagers and office...
sgpadmin
What do the terms ‘Tendonitis’ or ‘Tendinopathy’ sound like to you? It is needless to say th...
sgpadmin
Chronic pain is a condition in which pain stays for over 3 months as tissues heal over a prolonged t...
sgpadmin
Physiotherapy assists people of all ages suffering from injuries, medical conditions and illnesses t...
sgpadmin
Physiotherapy methods can make a world of difference for individuals suffering from pain and discomf...
sgpadmin
Lower back pain can be utterly debilitating and put a halt to one’s daily activities. Individuals ...
sgpadmin
Doctors often recommend physical therapy to patients who suffer from injuries, bone MUSCULOSKELETAL ...
sgpadmin
Physiotherapy essentially involves active and passive therapies as part of the multidisciplinary sci...
sgpadmin
What is physiotherapy? Physiotherapy is primarily an evidence-based allied health care profession pr...
sgpadmin
A physiotherapist is an expert caregiver, who is trained to restore your mobility, strength, and act...
sgpadmin
Any kind of hip and back pain can adversely affect walking hence people should not hesitate to seek ...
sgpadmin
Whether you are a trained athlete or a weekend player, there is always a risk of getting injured. Un...
sgpadmin
If you are a runner, you are probably going to suffer from sore legs. Hence, it is a good idea to op...
sgpadmin
The terms ‘Tendinopathy’ or ‘Tendonitis’ can baffle you if you are not from the medical back...
sgpadmin
Are you aware of the fact that every 1 in 3 elderly has a fall? Not only falls can lead to severe in...
sgpadmin
Shockwave has been used in treating various tendinopathies since the 1990s, however, there has been ...
sgpadmin
Physical therapy could help seniors maintain their independence, whether they are managing a long-te...
sgpadmin
Whether you suffer pain from arthritis, cancer treatments, fibromyalgia, or an old injury, you need ...
sgpadmin
Rare bumps and bruises can be expected when kids play sports, however, more than 1.35 million childr...
sgpadmin
Parent’s first priority should be Athlete safety, coaches, and players of all sports, from youth r...
sgpadmin
Strains and Sprains are the most common type of sports injury, and can take place in nearly every ty...
sgpadmin
Sports injuries have side-lined a lot of athletes for games and careers. Injuries can often occur wh...
sgpadmin
Elbow pain is very common which has a number of disorders which could be the cause. Elbow disorders ...
sgpadmin
Low back pain is generally defined as pain, muscle tension or stiffness. Low back strain is usually ...
sgpadmin
The Tensor Fasciae Latae (TFL) is a small but highly reactive muscle that serves as a cornerstone of...
sgpadmin
Sciatica is the symptom of pain down the leg which is experienced due to a low back problem. The sc...
sgpadmin
Muscle strain is an injury to a muscle as a result of a persistent activity. Virtually anyone can pu...
sgpadmin
Chronic pain is a long-term pain that lasts more than 12 weeks. The physical effects of chronic pain...
sgpadmin
There are five impressive health benefits of Rolfing: Improves Athletic Ability Rolfing upturns the ...
sgpadmin
Back pain is a common problem that will affect most people at some point in their life. The most com...
sgpadmin
Sprains A tear or stretch of the tissue connecting two bones (the ligament) is known as a sprain. Li...
sgpadmin
For patients going through breast cancer treatment, acupuncture is a brilliant form of therapy to he...
sgpadmin
Neurological rehabilitation is a supervised program for people with disorders relationg to the nervo...
sgpadmin
Here at Southgate Physio, our physiotherapists provide specialist treatment for a range of condition...
sgpadmin
Spine and back pain can be difficult to deal with, causing stiffness, limited range of motion and it...
sgpadmin
We at Southgate Physio are committed to provide you treatment facilities and rehabilitative care usi...
sgpadmin